Lingard Private innovates with Australia-first wearable device rehabilitation pilot
Healthe Care's Lingard Private Hospital has announced its orthopaedic pilot program – the first of its kind in Australia. It has the potential to streamline pre and post-operative rehab outcomes, while generating real time PROMs to gauge patient satisfaction.
To provide greater transparency on the patient care we provide, Healthe Care now publishes group patient reported experience measures (PREMs) and patient reported outcome measures (PROMs) on healthecare.com.au. This shows how our hospitals perform against, and in most cases, exceed industry standard, and in the near future we will also move towards publishing hospital specific data.
With our ongoing commitment to innovation and treatment ‘firsts’, Lingard Private has announced its orthopaedic pilot program – the first of its kind in Australia.
Not only does it have the potential to streamline pre and post-operative rehab outcomes – it also generates real time PROMs to gauge patient satisfaction.
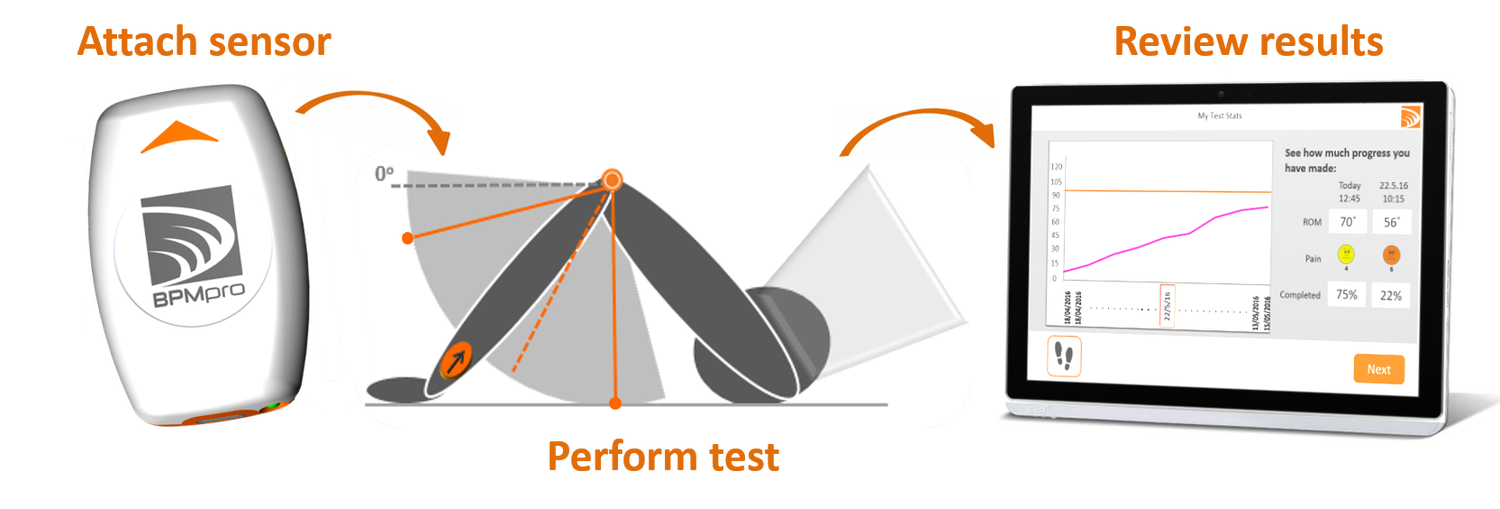
With the BPMpathway wearable device, medical-grade technology is provided for clinicians to remotely assess patient recovery on a daily basis. Dr Jonathan Young, Consultant Orthopaedic Surgeon at six Hunter Region hospitals including Lingard Private, and Director of Orthopaedics for Hunter New England Health is leading the Lingard Private pilot which, currently, is trialling total hips and total knees. In time, it may extend to shoulders and spine.
“The device and accompanying exercise programme have the potential to greatly enhance recovery after hip and knee replacement by giving patients updates on their progress and inspiring them to achieve the best outcome”, says Dr Young.
How does it work?
Following orthopaedic surgery, patients are supplied a wearable device to continue rehabilitation program in- home, without having to attend hospital. This is the first TGA approved wearable device, used for the first time in Australia. It connects via Bluetooth to the patient’s iPad or tablet, and worn while the patient undertakes range of motion exercises with pre-set parameters and end points, as part of their rehabilitation plan.
Via the device, results are sent to the patient’s surgeon and/ or physiotherapist, to remotely monitor post-operative care. Patients can also provide verbal feedback on pain points, and if their progress is not reaching post-surgical expectations, pre-set triggers automatically notify the specialist to arrange an in-person consultation. If all is going well, patients can continue their program remotely.
What are the benefits?
- The device is extremely beneficial for pre-operative (prehab) planning and determining baseline motion data, helping patients to immediately progress to post- operative care while continuing therapy
- Measurability of this tool enables us to assess different surgeries, post-operatively with regards to range of motion
- A more efficient model of rehabilitation with greater patient outcomes and engagement may be possible
What’s next?
Lingard will commence a 30 patient pilot before Christmas, initially for total hips and total knees. Subject to outcomes, this may extend to shoulder and spine.
On completion of the pilot, consideration will be given to how this integrates with the hospital, and the parameters for applying for study with a larger patient cohort.
Visit lingardprivate.com.au